Winek Research Group
Microbiome in Stroke and Aging
“The role of the infinitely small in nature is infinitely great.”
Louis Pasteur
Neurological disorders, common in the elderly, are a major cause of disability as well as a leading cause of death, and ischemic stroke is one of the main contributors to this disease burden. Not surprisingly, injury to the brain has consequences for other organs in the body, ultimately impacting the outcome after a stroke.
Orchestrated immune reaction follows stroke
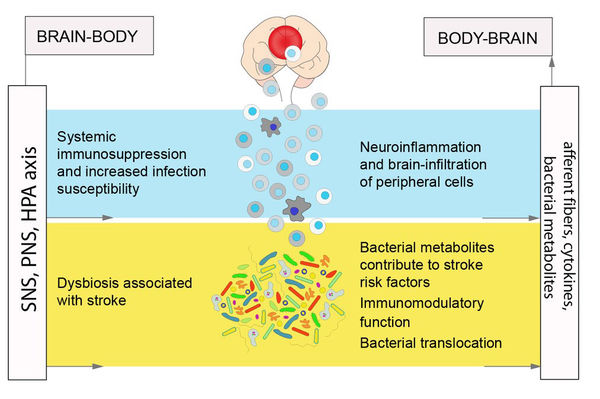
One of the important players in the response to an ischemic lesion in the central nervous system (CNS) is the immune system. A stroke induces an orchestrated immune reaction, including the infiltration of immune cells into the brain, followed by systemic immunosuppression. These peripheral immune cells contribute to tissue damage in the CNS, but also aid in repair processes, depending on the cell type and time point after the stroke.
Microbiome as a regulator of the immune system
Simultaneously, the systemic suppression of immune functions, potentially protective for the brain, increases susceptibility to infectious complications, leading to a worsening of the outcome. Intriguingly, the commensal microbial community, specifically gut microbiota, is also affected by the events after a stroke and may be a relevant modifier of the course and prognosis of illness, for example through its immunomodulatory actions.
Methods
In the search for new therapeutic targets and strategies, our group investigates the role of the microbiome and non-coding RNA regulators of the immune system in the pathogenesis and outcome of stroke. We work with in-vivo mouse and in-vitro cell culture models, RNA sequencing, FACS (fluorescence-activated cell sorting), MACS (magnetic-activated cell sorting), standard molecular biology techniques, and bioinformatic approaches. To increase the translational value of our studies, we plan close collaboration with clinical researchers.
Contact

Katarzyna Winek
Group Leader
+49 3641 65-6724
katarzyna.winek@~@leibniz-fli.de
Nicole Wolf
Assistance
+49 3641 65-6401
nicole.wolf@~@leibniz-fli.de